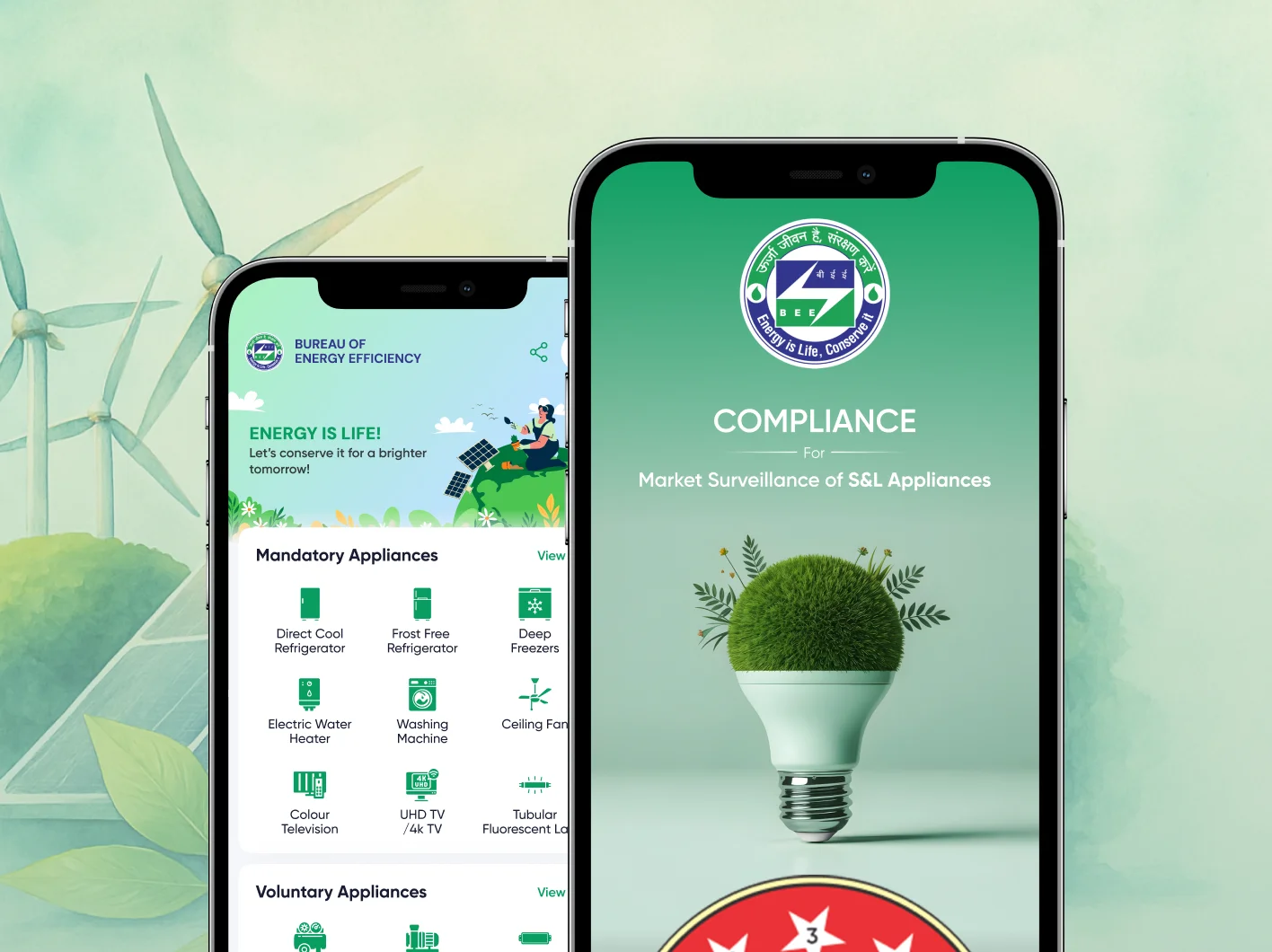
Transform your healthcare organization's financial performance with Webority's comprehensive revenue cycle management solutions. Our intelligent healthcare RCM software automates claims processing, reduces denials by 70%, and accelerates revenue collection through end-to-end workflow optimization—from patient registration to final payment reconciliation

-
AI AI Development
We engineer custom AI systems—from intelligent agents to scalable architectures—built for performance, security, and real-world impact.
 Industry AI Solutions
Industry AI SolutionsTailored AI solutions for healthcare, fintech, government, and enterprise—designed to solve sector-specific challenges with precision.
 AI Professional Services
AI Professional ServicesEnd-to-end AI services including consulting, governance, MLOps, and seamless integration to operationalize AI with confidence.

-
Services
- Custom Software Development
- Web Application Development
- Mobile Development
- UI/UX Design
- SaaS Product Development
- Blockchain Development
- MVP Development
- API Development & Integration
- Dedicated Development Teams
- Frontend Developers
- Backend Developers
- Mobile Developers
- Full-Stack Developers
- DevOps Engineers
- Engagement Models
- Salesforce Developers
- AI/ML Developers
INNOVATION AT SCALEWe turn ideas into powerful digital products—scalable, user-focused, and ready to disrupt markets.
 SKILL ON DEMAND
SKILL ON DEMANDAdd expert talent on demand. Our professionals integrate seamlessly to boost your delivery speed.
 STRATEGY MEETS EXECUTION
STRATEGY MEETS EXECUTIONSmart strategies, real impact. We align tech with your business goals to drive innovation.
 AMPLIFY YOUR REACH
AMPLIFY YOUR REACHFrom SEO to campaigns, we craft data-driven marketing that amplifies your brand’s reach.

-
Solutions
- Restaurant Management Solution
- Hotel Management System
- Cloud Kitchen App
- Cafe POS Customization
- Catering Management Platform
- Telehealth Software Development
- Hospital Management System
- Clinic Appointment System
- Online Pharmacy Platform
- Electronic Health Records
- Credentialing Platform
- Intelligent Medical Scribing
- Practice Management System
- Healthcare Billing & Invoicing
- Laboratory Management System
- Revenue Cycle Management
- Patient Engagement Portal
- School Management System
- College/University ERP
- Learning Management System
- Virtual Class + Live Sessions
- Exam Management System
- Online Course Marketplace
- Virtual Event Management
- Ticket Booking Portal
- Event Planning CRM
- Event Agenda & RSVP App
- Tour and Travel Website
DIGITAL DINING INNOVATIONSmart hospitality platforms bring together order management, guest engagement, and kitchen operations into a seamless digital flow. Restaurants, cafés, and hotels benefit from tools that accelerate fulfilment, reduce operational friction, and support personalisation at every touchpoint. As demand shifts throughout the day, these systems maintain speed, consistency, and quality—ensuring memorable dining moments for every guest.
 HEALTHCARE BEYOND BOUNDARIES
HEALTHCARE BEYOND BOUNDARIESWe help healthcare organizations modernize their services with secure, intuitive, and fully integrated digital platforms. Our solutions enhance patient engagement, streamline clinical and administrative workflows, ensure accurate and accessible health data, and empower providers to deliver efficient, high-quality care at scale
 SMART LEARNING TRANSFORMATION
SMART LEARNING TRANSFORMATIONEducation systems work best when academics, administration, and learning delivery sit on one connected platform. A unified digital setup helps schools and universities manage classes, assessments, communication, and daily operations with ease. Institutions gain better visibility, smoother coordination, and flexible learning environments that support students and teachers—both in classrooms and online—while keeping processes efficient and reliable.
 ENGAGING EXPERIENCES, ANYWHERE
ENGAGING EXPERIENCES, ANYWHEREEvent platforms built for modern audiences unify ticketing, scheduling, virtual participation, and audience interaction into an effortless, dynamic workflow. Organisers can coordinate large programs with precision, manage attendees in real time, and deliver rich experiences that feel immersive across both physical and digital venues. Whether small gatherings or global events, the system adapts seamlessly to ensure smooth execution and memorable engagement.
 MOBILITY MADE EFFICIENT
MOBILITY MADE EFFICIENTTransport and logistics operations benefit from connected platforms that improve routing, vehicle oversight, delivery tracking, and partner coordination. Centralised dashboards help teams manage schedules, reduce delays, and respond quickly to shifting demands. Automated processes enhance accuracy, optimise fleet utilisation, and strengthen reliability across the entire network—creating a streamlined, scalable foundation for efficient and timely movement of goods and people.
 POWERING DIGITAL COMMERCE
POWERING DIGITAL COMMERCEDigital commerce ecosystems thrive on platforms that support product discovery, multi-vendor operations, subscription models, and seamless checkouts. Scalable architectures enable fast browsing, personalised recommendations, and dependable fulfilment flows across diverse online stores. Brands gain the stability needed to grow, adapt to changing market patterns, and deliver smooth customer journeys—resulting in stronger engagement and higher long-term conversion.

- Case Studies
-
Resources
latest
Blogs

-
Company
WEBORITY
LEADERSHIP THAT DRIVES IMPACT
Our leadership team brings together decades of cross-industry expertise in technology, consulting, and digital transformation. With proven experience in scaling businesses, managing global delivery, and building innovative solutions, they provide the direction and clarity needed to navigate today’s complex business challenges. At Webority Technologies, leadership is not just about strategy—it’s about execution, accountability, and creating lasting value for our clients and teams.